Managing CF
Main Page

Cystic Fibrosis is complicated to manage. Click on a topic to read articles on airway clearance techniques, nutrition, updates on devices, or advice about CF complications.
Nutrition and CF
Good nutrition for a child or adult with CF means more than just eating a balanced, normal diet. A high-calorie diet containing all the essential nutrients without restriction on fat intake is recommended, along with pancreatic enzymes to control digestive symptoms, and supplemental fat-soluble vitamins: A, D, E, and K. To maintain weight, frequent and high-calorie meals and snacks are recommended.
What is a " good diet " for someone with CF?
Nutritional requirements for each person with CF are unique; there is no universal recommendation that applies to everyone. Requirements and recommendations depend on many factors including age, gender, severity of lung disease, malabsorption and the type of food a person likes. But there are some general recommendations for anyone with CF:
More Calories
Most people with CF have a higher caloric requirement than other individuals of the same age and sex because:
- More energy is used in breathing.
- Extra energy is used in fighting infections and during fevers.
- Fewer of the energy-producing nutrients in food are properly
digested and absorbed into the body, even when treatment is
optimal.
Research has shown that good nutrition is important for pulmonary function, and can contribute to a longer life expectancy.
Vitamins
Vitamins A,D, E, and K are known as the fat-soluble vitamins. These vitamins require an adequate amount of fat to be absorbed properly. Because people with CF can have problems with absorption of fat, it is important to replace these vitamins.
Pancreatic Enzymes
CF causes production of a thick mucus that plugs the duct leading from the pancreas to the small intestine. Consequently, the enzymes produced by the pancreas to help digest food cannot move into the small intestine. If left untreated, one result is malabsorption, an inability to properly absorb nutrients. To compensate for this enzyme shortage, many people with CF must take replacement pancreatic enzymes.
When Do I Take Enzymes?
Enzymes must be taken to help digest every meal and snack, except for snacks that are virtually free of protein, starch, and fat (such as apple juice). Studies show that enzyme preparations are equally effective when taken anywhere from a half-hour before to a half-hour after eating. That way, the enzymes are in the small intestine when needed.
What If I Can't Eat Enough Calories?
Some people with CF cannot take in enough calories by mouth to gain or maintain weight. For them, calories and all the essential nutrients can be given by tube feedings. Many achieve excellent nutrition through this method.
Is There Any Help With Nutritional Products?
The Scandipharm Comprehensive Care Program for CFTM provides free ADEKs® multivitamins, Scandishake® nutritional supplements, and Flutter® mucus-clearance devices to people taking Ultrase®. The program enhances Scandipharm's mission of improving the overall quality of care, while lowering its cost. For more information on this program, talk to one of the CF team members.
How Can I Manage CF and Nutrition?
The key to managing nutritional needs successfully is to match dietary needs to each individual:
- Assess individual needs
- Adjust for clinical status
- Factor in age-related needs
A comprehensive nutritional management plan developed jointly by the CF Team, the person with CF, and the family is needed.
Back to top
Pulmonary Function Tests
What are Pulmonary Function Tests (PFTs)?
 Pulmonary function tests are machine assessments of the performance of the lungs, measuring basic function and volume. Many of the tests are done in a special Pulmonary Function Laboratory. There are various computerized machines that answer very specific questions about lung function.
Pulmonary function tests are machine assessments of the performance of the lungs, measuring basic function and volume. Many of the tests are done in a special Pulmonary Function Laboratory. There are various computerized machines that answer very specific questions about lung function.
Some Common Tests:
Spirometry: tests done at every clinic visit to determine the vital capacity of the lungs. Spirometry measures the amount of air breathed and the speed at which it is blown out.
- SVC: (slow vital capacity)
- FVC: (forced vital capacity) This measures the volume of air that is blown out in a single maximum exhaled breath. It is inversely related to the amount of air trapped by obstruction. The worse the airway obstruction, the less the FVC.
- FeV1: (forced expiratory volume) This measures how fast the lungs can push air out in one second. Your result is measured against a predicted result, a mean of values in healthy people of the same sex, height, and weight. The result is written as the percent of the predicted result. The less air expired in the first second, the higher the level of airway obstruction.
Lung Volume Measurements: these indicate the size of the lungs and the amount of air remaining inside after exhalation
Exercise testing: Problems may become more apparent during exercise, therefore, sometimes PFTs are measured during treadmill or other exercise while heart and respiratory rates are monitored.
Blood oxygenation measures(ABGs): These indicate how effective the lungs are in bringing oxygen into the bloodstream and removing carbon dioxide from it.
What do these tests show in my lungs?
- How well my lungs are working
- If antibiotics are helping to clear up an infection
- If the current daily care program is adequate
How often should they be done?
- Spirometry is initiated at 5 or 6 years of age or whenever a child can understand the instructions and cooperate. After that, spirometry is done at every clinic visit so that the clinician can evaluate your progress.
Research is being done on methods to measure infants.
- Full PFTs are done on an annual basis. They are extremely accurate monitors of change in lung function, even when no new symptoms or signs have emerged.
How some of the spirometry tests are done:
A spirometer is a tube leading into a pneumotach which measures air flow and volume. The results are graphed and displayed on the computer monitor. In order to make accurate measurements, nose plugs are worn to close the nasal passages so that the air can only be blown out through the mouth.
- FVC: (forced vital capacity) After several slow deep breaths in, you breathe out as hard as you can for six full seconds. This measures the volume of air that is blown out in a single maximum exhaled breath.
- FeV1: (forced expiratory volume) After several slow deep breaths in, you blast all of the air out of your lungs as fast as possible in one long burst. This measures how fast the lungs can push air out in one second.
Back to top
Metered Dose Inhaler
What is a Metered Dose Inhaler (MDI)?
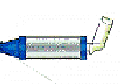
|
An MDI is device that sends a measured amount of medicine directly into the lungs. Sometimes it is used with a spacer to make it easier to use. The spacer can help to deliver the medicine to the lungs and lessen the bad taste of the medicine.
|
How do I use an MDI?
- Remove the cap and hold the inhaler upright.
- Place the spacer, if used, on the inhaler.
- Shake the inhaler.
- Tilt your head back a bit. Breathe in and breathe out. Then place the spacer or mouthpiece in your mouth.
- Press down on the inhaler to release the medicine. This is called one " puff ".
- Start breathing in SLOWLY.
- Hold your breath for 10 seconds to allow the medicine to reach deeply into the lungs.
- Repeat puffs as prescribed. If you can, try to wait a minute in between puffs.
|
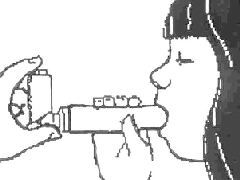
|
How to avoid common inhaler mistakes
- Breathe in and out BEFORE pressing your inhaler
- Inhale SLOWLY
- Breathe in through your mouth, not your nose
- If you are NOT using a spacer, start inhaling BEFORE pressing down on the inhaler, and keep inhaling as you press down
- Make sure you breathe in evenly and deeply
How to clean your inhaler
It is very important to clean your inhaler and spacer regularly. Without cleaning, a build-up can occur which will stop the medicine from being delivered.
- Once a week, wash the L-shaped mouthpiece and spacer in warm, soapy water. (If you have Intal or Tilade, do not get the canister wet!)
- Rinse thoroughly.
- Let dry COMPLETELY.
What else do I need to know?
It is important to monitor expiration dates and the amount of medication remaining.
How can I tell how much medicine is left?
- Shake the canister and listen for the sound of the remaining medication.
- If you can, keep track of how many puffs you take. Most canisters have about 200 puffs.
- If you want to check how much medicine is left in the canister, place it in a glass or bowl of water. Watch how it floats in the water. (This method will NOT work for Intal or Tilade. These canisters cannot get wet.)
InspirEase and E-Z Spacer
These spacers are especially helpful in delivering medications to children. After attaching the medication canister and pressing down, medicine is released into a bag which collapses when the child breathes in. Here are the steps to using the InspirEase. Be sure to read the directions that come with your spacer.
- Connect the mouthpiece to the reservoir bag.
- Untwist the reservoir bag to open it fully. Shake the canister and place it in the opening by the mouthpiece.
- Place fingers on the canister or on the fingerholds of the actuation aid and pull down to release one dose (one puff).
- Breathe in slowly (if you hear a whistle sound, you are breathing too fast!). The bag will collapse as the medication is inhaled.
- If possible, have the child hold his/her breath before exhaling
- Repeat as directed.
Back to top
Nebulizers
What is a nebulizer?
A nebulizer is a device driven by a compressed air machine that changes a liquid medicine into a mist so it can be breathed into the lungs. It consists of a cup, a mouthpiece attached to a T-shaped part or a mask, and thin, plastic tubing to connect to the compressed air machine.
Important points to remember:
There are many different types of nebulizers available, so always follow the instructions that are provided with your machine.
It usually takes about 10 minutes to complete a nebulized treatment.
The liquid medicine must be stored as directed.
The nebulizer MUST be cared for after each use. Cleaning gets rid of germs that can cause infections, and it also keeps the nebulizer from clogging up.
Thorough DRYING of all of the parts after cleaning is essential.
How to use a nebulizer
- If your medicine is NOT premixed: Using a clean dropper, measure the right amount of saline and place into the nebulizer cup. Then, with a different dropper, measure the right amount of medicine and place into the cup. Be sure not to confuse the two droppers.
- If your medicine is premixed, measure the correct amount and place into the nebulizer cup.
- Connect the mouthpiece to the T-shaped part and then fasten this to the cup. If your child is less than 2 and you are using a mask, fasten this to the cup.
- Put the mouthpiece into the child's mouth between the teeth and sealed lips. Or place the mask on the child's face.
- Turn on the nebulizer.
- Take slow, deep breaths through the mouth.
- If possible, hold each breath for 1-2 seconds.
- Continue slow breathing for 10 minutes, or until the medicine is gone.
- Care for the nebulizer after each use paying close attention to the thorough DRYING of all parts.
Caring for your nebulizer
After each use: rinse
- Remove the mask or mouthpiece and T-shaped part from the cup.
- Remove the tubing and set it aside. The tubing should not be washed or rinsed.
- Rinse the mask or mouthpiece and T-shaped part in warm running water for 30
seconds. Use distilled or sterile water for rinsing, if possible.
- Shake off excess water. Air dry COMPLETELY on a clean cloth or paper towel.
- Put the mask or mouthpiece and T-shaped part, cup, and tubing back together, and connect the device to the compressor. Run the machine for 10 to 20 seconds to dry the inside of the nebulizer.
- Disconnect the tubing from the compressor. Store the nebulizer in a sealable plastic bag.
- Place a cover over the compressor.
Once every day: wash
Wash the mask or mouthpiece and T-shaped part with a mild dishwashing soap and hot water. If your manufacturer's instructions allow, you may use an automatic dishwasher. Rinse well.
Once or twice a week after washing and rinsing: disinfect
- Wash your hands
- Read and follow the manufacturer's instructions on disinfection. If the manufacturer's instructions allow, disinfect the nebulizer using one of these options:
- Boil for 5 minutes
- Microwave (in water) for 5 minutes
- Dishwasher (water temperature above 158�) for 30 minutes
- Soak in a solution of 1 part household bleach and 50 parts water for 3 minutes
- Soak in 70% isopropyl alcohol for 5 minutes
- Soak in 3% hydrogen peroxide for 30 minutes.
Do not use a nebulizer that cannot be disinfected using one of these options.
- Rinse the nebulizer parts and the eyedropper or syringe under warm running water for 1 minute. Use sterile water for the last rinse. To make sterile water, boil it for 5 minutes. (If you disinfect by boiling, you do not need to rinse the nebulizer.)
- Shake off the water and air dry COMPLETELY on a clean cloth or paper towel.
- Put the mask or mouthpiece and T-shaped part, cup, and tubing back together, and connect the device to the compressor. Run the machine for 10 to 20 seconds to dry the inside of the nebulizer thoroughly.
- Disconnect the tubing from the compressor. Store the nebulizer in a sealable plastic bag.
- Clean the surface of the compressor with a well-wrung, soapy cloth or sponge. You could also use an alcohol or disinfectant wipe. NEVER PUT THE COMPRESSOR IN WATER.
- Place a cover over the compressor.
Back to top
Measuring Peak Flow
What is a Peak Flow Meter?
A peak flow meter is a simple device that measures the amount of air you are able to exhale quickly. This can help show whether your airways are constricted (narrowed). If you can expel a lot of air quickly, your bronchial tubes are open. Regular peak flow monitoring can sometimes detect loss of lung function even before you notice the symptoms.
How to Take a Peak Flow Reading
- Set the peak flow meter at zero.
- Stand up tall.
- Take a very deep breath.
- Place the mouth piece in your mouth between your teeth and close your lips around it.
- Blow out your mouth as hard and fast as you can (1-2 seconds).
- Be sure not to cough or put your tongue on the mouth piece.
- Look at the number indicated and write it down.
- Repeat steps 1-7 two more times (3 times total).
- Write down the highest number on your Peak Flow Diary.
How to Care for Your Peak Flow Meter
If it is dirty, rinse it with warm water.
Shake out all of the water and let it dry on a towel.
Make sure it is dry before you use it again.
Keep it in a safe place, and don't let other kids play with it.
Back to top
If Your Child Is Sick
 All children occasionally get sick. It is usually OK to first try common remedies such as
All children occasionally get sick. It is usually OK to first try common remedies such as
- Drink additional fluids
- Get adequate rest
- Treat low grade fevers (Usually up to 101 degrees Fahrenheit, but check with your physician)
- Maintain weight by eating small frequent meals and snacks
- Understand and use the medicines prescribed regularly
- Increase chest percussion
But sometimes you need more help. Please call your physician for any of the following:
- Chest pain or acute shortness of breath
- Fever above 100 degrees Fahrenheit for more than a few days
- Blood in sputum or stool
- Diarrhea, constipation, or abdominal cramping
- Vomiting
- Notable change in activity for more than a few days
- Signs of a respiratory infection in a young child (increased cough, elevated temperature, or other signs of a cold)
- Weight loss of five pounds or greater, or a rapid weight gain
- Swollen ankles, hands, or feet
Back to top
Handwashing: Your Mother Was Right
" Hand washing is the single most effective way to prevent the spread of communicable diseases ", Center for Disease Control
Why is hand washing important?
The most important thing that you can do to keep from getting sick is to wash your hands.
By frequently washing your hands you wash away germs that you have picked up from other people or from contaminated surfaces.
What is good hand washing technique?
There is more to hand washing than you think! By rubbing your hands vigorously with soapy water, you pull the dirt and the oily soils free from your skin. The soapy lather suspends both the dirt and the germs trapped inside. And then the rinse water quickly washes it all away.
Here's how to do it:
- Wet your hands with warm running water.
- Add soap, then rub your hands together, making a soapy lather.
Rub your hands together, being careful to rub all of the surfaces, for about 15 seconds.
HINT: Singing a quick chorus of "Row, Row, Row Your Boat"
will keep you rubbing for the full 15 seconds!
- Do this away from the running water, being careful not to wash the lather away
- Wash the front and back of your hands,as well as between your fingers and under your nails.
- Rinse the soap off under running water.
- Use a paper towel to turn off the faucet in a public place.
- Dry your hands thoroughly.
HINT: Carry alcohol-based hand washing gels
for places where you don't have access to soap and water.
Back to top
Cystic Fibrosis Related Diabetes
What Is It?
Diabetes is a disease that may occur in a person with Cystic Fibrosis because of
- damage to the pancreas from CF
- decreased sensitivity to insulin
- or genetic factors
Fibrosis of the " endocrine " part of the pancreas can gradually lead to impaired function of specialized pancreatic cells, the insulin-producing islet cells. Insulin is a hormone critical to the body's ability to regulate blood sugar levels. (CF affects the " exocrine " portion of the pancreas, but prolonged damage may affect rest of the pancreas.)
What Happens?
People may become glucose intolerant, that is, less able to clear glucose from the bloodstream. The body is then unable to use or store food effectively; so the blood sugar level rises and can cause damage to many parts of the body.
How Would I Know if I Had It?
There may be no noticeable symptoms. Random blood or urine glucose levels may be normal.The oral glucose tolerance test (OGTT) is the most reliable method of identification. This test involves drinking a glucose (sugar) solution and measuring blood glucose at baseline and two hours later. This test should be considered for CF patients over the age of 16 on an annual basis.
What Can Be Done if I Develop Diabetes?
Management usually includes dietary modification in order to regulate the types of food eaten and the timing of food intake. In addition, insulin or oral medications may be given to lower blood sugar. Blood glucose values can be monitored at home to determine if the glucose levels are acceptable.
Back to top
Vascular Access Devices
Vascular access devices are tools designed for the administration of medications, I.V. fluids, parenteral nutrition solutions, and blood products. They can also be used to take a blood sample. Some are totally implanted, such as ports, and can remain in the body for 3-5 years. Others, such as PICC lines and tunneled catheters, can be seen and accessed from the surface of the body.
Why have a vascular access device?
After repeated courses of intravenous medications, veins may become scarred, and it may become more and more difficult to find veins suitable for blood tests and administration of medication. Several different devices and procedures have been developed to provide improved access to veins.
Who should consider vascular access?
- Those who require repeated courses of intravenous antibiotics
- Those who have problems finding suitable veins
- Those whose IVs are not lasting very long
Some common types of vascular access devices
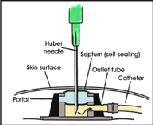
Implanted port
|
Implantable ports:
This small device (about the diameter of a quarter and about a half inch thick) is completely under the skin, and out of the way. You will still feel a small bubble, however. It is connected to a catheter (a small flexible tube) that is placed in a large vein within the chest. You can also feel the catheter tunneled under the skin until it enters the vein.
|
These catheters need to be flushed at least once a month. They usually last about 3-5 years.
Disadvantages:
- There is some pain when the access needle pierces the skin to get into the bubble. This can be minimized with Emla cream.
- These devices must be placed by and removed by physicians.
Other names of ports: Mediport, BardPort, Med-Port, Infusa Port, Port-a-Cath, P.A.S. Port (this usually goes into a vein in the arm).
Tunneled Central Venous Catheters (TCVC):
The advantage of these catheters is their larger diameter, which is helpful for situations where good blood flow is required.
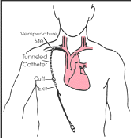
Tunneled catheter
|
The TCVC is inserted into the vascular system, then a portion of the tubing is tunneled through the subcutaneous space and exited through the skin at a convenient location on the chest. A dacron cuff just above the exit site acts as a barrier against infection and prevents the catheter from slipping out.
|
Disadvantages: The catheter extends several inches outside the body and needs periodic flushing. The exit site must be dept very clean to avoid infection and the dressing must be changed at least twice a week, more often if wet.
Other names of Tunneled Central Venous Catheters: Hickman, Broviac.
PICC Lines:
Peripherally Inserted Central Venous Catheters (PICC) consist of a thin plastic line that is placed into one of the large antecubital veins (inner elbow area, where blood is commonly drawn) and is threaded into the superior vena cava above the right atrium of the heart. What's nice about this catheter is that it doesn't require a surgeon to insert - an IV nurse can do it. It can also be removed by a nurse. The catheter can stay in for as long as a year. Disadvantages: The catheter needs to be flushed about once a week, if not used. With repeated use, veins can become scarred and unusable. An x-ray is needed to check the placement of a centrally placed line.
Landmark catheter:
A short catheter (3-6 inches long) that is placed into the vein with a needle. It is usually placed in the lower arm or inside the elbow. Landmark catheters usually last up to several weeks. Usually does not require an x-ray afterwards for placement.
Back to top
Maintaining an Implanted Vascular Access Port
Vascular access ports are totally implantable devices that permit the infusion of medications, parenteral nutrition solutions, blood products and other fluids; ports are also useful for blood sampling. Implanted ports were developed to help provide reliable vascular access for patients who require long-term drug or fluid therapy. Ports are available in a variety of materials and designs; some maintenance is required to use these devices.
Flushing a port during intermittent infusions:
During intermittent infusions, use 5cc's of Heparin ( 10 U/cc) to flush a port.
Flushing a port that is not being accessed:
When not accessed, ports are flushed once a month with 5 cc's of Heparin
( 100 U/cc). The exception to this is a Groshong Implanted Port which is flushed monthly with 10cc's of Heparin ( 100 U/cc).
Site preparation prior to flushing:
Application of EMLA cream to numb the site 1 hour before access is highly recommended.
PORT ACCESS IS A STERILE PROCEDURE. Ports may be accessed only with a non-coring (Huber) needle. Care must be taken to follow accessing instructions carefully.
Equipment needed:
- Non-coring (Huber) needle of the proper size. Use 22g x 1 inch if unsure.
- Normal saline
- Heparin flush solution 10u/cc
- 12cc syringes with needles
- Alcohol preps
- Sterile gloves
- Sterile field
- 3 Persist swabs
- Biopatch
- TegadermHP Transparent Dressing
- 3 packages 2x2's
- Tape
- Extra needles, 25 gauge 5/8"
- Injection cap
- Safety pin
Instructions:
- Wash your hands
- Palpate the port until you have identified the silicone plug in the center and the metal ring which surrounds it. Be sure you can stabilize the port between your first and second fingers in order to access it.
- Place your supplies on a clean surface which has been wiped with alcohol and allowed to dry.
- Remove top from sterile saline vial.
- Arrange your supplies on the sterile field.
- Wash your hands again and don sterile gloves.
- Draw up saline using sterile technique.
- Flush the non-coring needle and tubing with the saline.
- Clean skin spiraling outward to 3 inches using three Persist swabs. Do not bring the swab back to the center after you are done.
- Palpate the port until you have identified the landmarks as above.
- If the patient has sensitive skin, remove Persist with alcohol or normal saline.
- Stabilize the port firmly between the first and second fingers of your non-dominant hand. Put the thumb of your dominant hand directly over the needle and push it firmly into the port until you feel the needle hit the back of the port. Aspirate for blood return.
- Flush with 5-10 cc normal saline using a pulsing motion and leaving positive pressure in the port. Heparin lock with heparinized saline 10U/cc if port will be deaccessed and not used.
- Place the Biopatch around the needle, grid side up.
- If you are using a winged needle, place about 2-3 folded 2x2's under the needle wings to stabilize it. If you have a gripper needle, you won't need to place 2x2's under the needle.
- Cover the site with the transparent dressing leaving half the T-Port outside the dressing. Loop the exposed tubing and tape on top of the dressing. If you have an IV infusion running, place some tape around the IV tubing close to the port, and pin the tubing to the shirt. (Take care not to puncture the IV tubing).
- Document the size of the access needle and patient tolerance of the procedure. Date and initial the dressing.
Conditions to Watch For:
The site should remain clean and dry. If a port dressing becomes wet or soiled, change the dressing immediately. Watch the site carefully for any signs or symptoms of infection/phlebitis.
Possible complications:
VENOUS THROMBOSIS: a clot can form around the catheter
- Pain in the arm, neck, and/or shoulder which is noted on the same side of the body as where the port is inserted.
- Swelling may be noted above the clavicle, neck, and/or face.
CATHETER CLOTS: the catheter becomes blocked.
If the pump reads occlusion or high pressure and you have checked to make sure that there are no kinks in the line or the clamp is not on, try to flush the line with normal saline. If it flushes sluggishly, gently heparin lock the line and call the MD.
AIR EMBOLISM:
- Patient may feel chest pain or pain with deep inspiration.
- Shortness of breath or breathing rate increases.
- Skin may appear pale of blue colored around the lips and nailbeds.
- Coughing noted.
CATHETER EMBOLUS: A piece of the catheter may tear off and enter the blood stream.
- Patient may feel dizzy or faint.
- Patient may have chest pain, especially with deep inspiration.
- Patient may have shortness of breath and breathing rate increases.
- Skin may appear pale, or blue color may be noted around the lips and nailbeds.
Back to top
Main Page
 Pulmonary function tests are machine assessments of the performance of the lungs, measuring basic function and volume. Many of the tests are done in a special Pulmonary Function Laboratory. There are various computerized machines that answer very specific questions about lung function.
Pulmonary function tests are machine assessments of the performance of the lungs, measuring basic function and volume. Many of the tests are done in a special Pulmonary Function Laboratory. There are various computerized machines that answer very specific questions about lung function.