 |
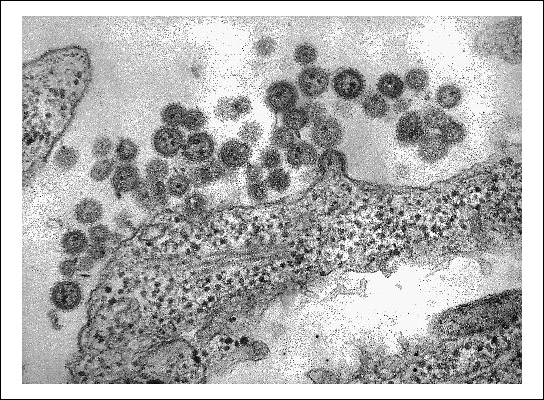
Machupo |
http://www.idph.state.il.us/Bioterrorism/vhf_a.htm
Epidemiology and History:
Beginning in 1959 and continuing through the early 1960’s, outbreaks of Bolivian hemorrhagic fever occurred in rural areas throughout Bolivia, including the Beni department and the areas surrounding San Joaquin near the eastern frontier of Bolivia. In San Joaquin, the rapid spread and gruesome death of villagers suffering from the fever led to widespread panic, prompting Bolivian authorities to request assistance from US scientists. Bolivians referred to the mysterious disease as “Black Typhus” alluding to the hemorrhaging, high fever, pain, and rapid death caused by the illness. After months of investigation, US government isolated the Machupo virus from the Arenavirus family as the cause of the outbreaks. To study the disease in rural Bolivia, Karl Johnson from the NIH had developed a portable laboratory glove box to house research mice in sterile conditions. During the identification process, several virologists became ill and nearly 20% of the San Joaquin villagers died of the disease. Since then, isolated outbreaks of Machupo have occurred throughout rural eastern and northern Bolivia, where the virus is endemic.
http://eee.uci.edu/clients/bjbecker/PlaguesandPeople/week10d.html
Transmission:
Machupo virus is spread through aerosolized, food-borne, or direct contact of virus particles. These particles result from the saliva, urine, or feces of Calomys callosus, the field mouse reservoir of the virus. In San Joaquin, the virus spread most effectively when the dried mouse urine on the dirt floors of homes was swept into the air during cleaning and inhaled by inhabitants of the home. Outbreaks of Machupo occur when a sudden population or human contact increase in the rodent population is prompted by abundant food sources or human living and farming patterns. Few reports of person-to-person spread of the virus have been reported including among nursing and laboratory staff and family members of an infected individual.
Diagnosis:
Symptomatic diagnosis of Machupo is difficult given its similarity to other arenavirus-caused hemorrhagic fevers, including Junin and Sabia, as well as other endemic diseases like dengue, malaria, and yellow fever. The best prospects for rapid diagnosis are educating health care providers to increase rapid recognition of Bolivian hemorrhagic fever. In a BS-4 laboratory, the virus can be identified through rapid enzyme-linked immunosorbent assays for antigen and IgM antibodies. There are also some inexpensive reagents, such as Triton X-100, which could reduce viral titers to a level enabling real time testing capability.
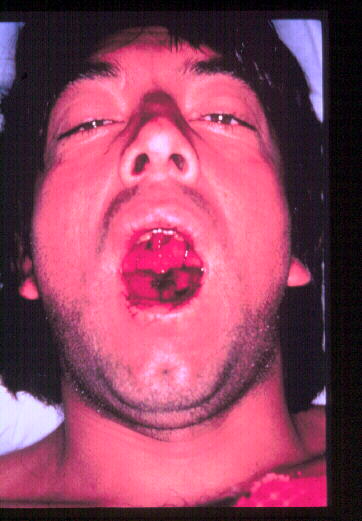
Symptoms:
Preliminary symptoms of Bolivian hemorrhagic fever caused by the Machupo virus include fever, headache, fatigue, myalgia, and arthralgia. In some patients, hemorrhagic signs develop, including bleeding from nasal and oral mucosa, as well as the bronchopulmonary, gastrointestinal, and genitourinary tracts. A few patients develop neurological symptoms such as tremors, loss of muscle control, and seizuring. Death can occur between a few hours and a few days after the onset of symptoms. Symptoms generally last for one week after a one week incubation period.
www.telemedicine.org/biowar/bw26.jpg
Treatment:
Like many arenaviruses, Machupo is responsive to intravenous
ribavirin given to patients with symptoms meeting a clinical case definition
and laboratory confirmation of Machupo. Additionally, the vaccine for Argentinean
hemorrhagic fever (cased by the genetically-similar Junin virus) appears to
provide a level of cross-protection against Machupo and may become a preventative
measure for high-risk individuals. The most effective means of controlling
the virus is to eliminate contact between humans and mice through trapping,
territory monitoring, and elimination of rodent food sources.